What Causes Cuboid Syndrome?
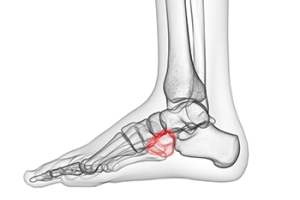
 Cuboid syndrome is a condition in which the cuboid bone, located in the center of the foot, becomes dislocated. This produces symptoms such as foot pain, difficulty walking, swelling, sensitivity, and a reduced range of motion of the foot or ankle. The symptoms are like a sprain. Although the precise cause of cuboid syndrome is unknown, this condition is thought to arise from a forceful turn of the cuboid bone outwards as the heel bone turns inwards. This can be caused by an ankle sprain or other lower limb injury. Certain factors can increase the likelihood of cuboid syndrome. These include instability in the midfoot, being overweight or obese, wearing ill-fitting shoes or poorly constructed orthotics, and training excessively or on uneven surfaces. If you are experiencing the symptoms of cuboid syndrome, schedule an appointment with a podiatrist near you.
Cuboid syndrome is a condition in which the cuboid bone, located in the center of the foot, becomes dislocated. This produces symptoms such as foot pain, difficulty walking, swelling, sensitivity, and a reduced range of motion of the foot or ankle. The symptoms are like a sprain. Although the precise cause of cuboid syndrome is unknown, this condition is thought to arise from a forceful turn of the cuboid bone outwards as the heel bone turns inwards. This can be caused by an ankle sprain or other lower limb injury. Certain factors can increase the likelihood of cuboid syndrome. These include instability in the midfoot, being overweight or obese, wearing ill-fitting shoes or poorly constructed orthotics, and training excessively or on uneven surfaces. If you are experiencing the symptoms of cuboid syndrome, schedule an appointment with a podiatrist near you.
Cuboid syndrome, also known as cuboid subluxation, occurs when the joints and ligaments near the cuboid bone in the foot become torn. If you have cuboid syndrome, consult with the foot specialists from Podiatry Associates of Belleville. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Cuboid syndrome is a common cause of lateral foot pain, which is pain on the outside of the foot. The condition may happen suddenly due to an ankle sprain, or it may develop slowly overtime from repetitive tension through the bone and surrounding structures.
Causes
The most common causes of cuboid syndrome include:
- Injury – The most common cause of this ailment is an ankle sprain.
- Repetitive Strain – Tension placed through the peroneus longus muscle from repetitive activities such as jumping and running may cause excessive traction on the bone causing it to sublux.
- Altered Foot Biomechanics – Most people suffering from cuboid subluxation have flat feet.
Symptoms
A common symptom of cuboid syndrome is pain along the outside of the foot which can be felt in the ankle and toes. This pain may create walking difficulties and may cause those with the condition to walk with a limp.
Diagnosis
Diagnosis of cuboid syndrome is often difficult, and it is often misdiagnosed. X-rays, MRIs and CT scans often fail to properly show the cuboid subluxation. Although there isn’t a specific test used to diagnose cuboid syndrome, your podiatrist will usually check if pain is felt while pressing firmly on the cuboid bone of your foot.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are ice therapy, rest, exercise, taping, and orthotics.
If you have any questions, please feel free to contact our office located in Belleville, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Cuboid Syndrome
Cuboid syndrome mostly affects athletes, although it can affect non-athletes too. It is also known as cuboid subluxation or cuboid fault syndrome. This condition occurs when joints and ligaments near the cuboid bone of the foot are damaged, or when the cuboid bone itself is dislodged from its natural position. It is usually marked by pain on the outer side of the foot, which may be persistent or may come and go. Cuboid syndrome can be difficult to diagnose unless it becomes severe and more noticeable. Your doctor will likely ask questions about when the pain began and how long it has been present, and will put pressure on the cuboid bone to determine if that area is the origin of the pain.
Causes of Cuboid Syndrome
- Any repetitive stresses placed on the foot due to athletic activities are a common cause of cuboid syndrome.
- Although it develops over time, it is possible that this syndrome can occur all of sudden due to a single event or injury.
- Over-pronation can exacerbate the condition if not corrected.
Disagreements Amongst Podiatrists Regarding Cuboid Syndrome
- Some refer to it as the dislocation of the calcaneal-cuboid joint only.
- Other podiatrists see it as an injury of the ligaments located nearby, which also involves the cuboid bone.
It is very important that when you experience any kind of pain on the side of your foot, you should seek medical care right away. If a subluxed cuboid is caught early, your feet may respond well to the treatment, and you can get back into sports or other activities again as soon as the pain subsides.
Treating the Causes of Plantar Fasciitis
 Plantar fasciitis is a common injury in which the plantar fascia, a ligament that runs along the bottom of the foot and connects the heel bone to the toes, becomes overstretched and inflamed. When it comes to treating this condition, the first step is to determine what has caused the plantar fascia to overstretch. Sometimes this is caused by overpronation, a walking pattern common in people with flat feet in which the foot rolls too far inwards. It may also be caused by unusually high arches in the midfoot. These issues can both be corrected using orthotics. When plantar fasciitis is caused by overuse from playing sports, running, or frequently doing exercises that put stress on the feet, taking time to rest and recover, ensuring that you are wearing the appropriate shoes, and losing excess weight can all potentially help relieve symptoms. If you are suffering from heel or arch pain, it is suggested that you seek the care of a podiatrist.
Plantar fasciitis is a common injury in which the plantar fascia, a ligament that runs along the bottom of the foot and connects the heel bone to the toes, becomes overstretched and inflamed. When it comes to treating this condition, the first step is to determine what has caused the plantar fascia to overstretch. Sometimes this is caused by overpronation, a walking pattern common in people with flat feet in which the foot rolls too far inwards. It may also be caused by unusually high arches in the midfoot. These issues can both be corrected using orthotics. When plantar fasciitis is caused by overuse from playing sports, running, or frequently doing exercises that put stress on the feet, taking time to rest and recover, ensuring that you are wearing the appropriate shoes, and losing excess weight can all potentially help relieve symptoms. If you are suffering from heel or arch pain, it is suggested that you seek the care of a podiatrist.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact the foot specialists from Podiatry Associates of Belleville. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Belleville, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Ankle Pain From Synovitis
 The ankle is a hinged joint formed by the tibia and fibula bones in the lower leg and the talus bone at the top of the foot. Like other joints in the body, the ankle joint is lined by the synovium, a tissue that allows the joint to move smoothly. When the synovium becomes inflamed, a condition called synovitis develops. This condition is associated with gout and rheumatoid arthritis, but can also be caused by a sudden injury or repetitive overuse of the ankle. Synovitis may lead to redness, swelling, and warmth in the ankle joint, as well as pain in the front or along the sides of the ankle. This can make walking very difficult. If you are experiencing the symptoms of ankle synovitis, it is suggested that you see a podiatrist, who can diagnose and treat your condition.
The ankle is a hinged joint formed by the tibia and fibula bones in the lower leg and the talus bone at the top of the foot. Like other joints in the body, the ankle joint is lined by the synovium, a tissue that allows the joint to move smoothly. When the synovium becomes inflamed, a condition called synovitis develops. This condition is associated with gout and rheumatoid arthritis, but can also be caused by a sudden injury or repetitive overuse of the ankle. Synovitis may lead to redness, swelling, and warmth in the ankle joint, as well as pain in the front or along the sides of the ankle. This can make walking very difficult. If you are experiencing the symptoms of ankle synovitis, it is suggested that you see a podiatrist, who can diagnose and treat your condition.
Ankle pain can have many different causes and the pain may potentially be serious. If you have ankle pain, consult with the foot specialists from Podiatry Associates of Belleville. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendinitis
- Achilles tendon rupture
- Stress fractures
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions, please feel free to contact our office located in Belleville, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ankle Pain
The ankle joint is the point at which the bones of the leg and foot join. This joint is crucial because it is responsible for the foot’s mobility. Ankle pain is typically the result of inflammation from an injury to bones, joint space, cartilage, ligaments, tendons, or muscles in the area. Commonly associated symptoms with ankle pain are bruising, redness, numbness, stiffness, weakness, and tingling.
The most common causes of ankle pain are sprains and injuries. Ankle sprains are one of the most common musculoskeletal injuries. Sprains occur when the ligaments of the ankle become partially or completely torn due to sudden stretching. Sprains can occur on either the inner or outer sides of the ankle joint. Usually, these injuries occur when the ankle is twisted in an activity by stepping off an uneven surface. More specific causes include rheumatoid arthritis, gout, osteoarthritis, and Achilles tendonitis.
If you are experiencing ankle pain, you should consult with your podiatrist to choose the best method of care. Your doctor will conduct an examination of your ankle to determine the underlying cause of the pain.
Are Bunions Affecting Your Everyday Life?
Topical Treatments for Diabetic Foot Wounds
Those with diabetes may find that their feet are more prone to dryness, itchiness, bruising, cuts, scrapes, and sores. These seemingly minor issues can be dangerous for diabetic feet. Even small wounds may heal slowly and poorly, becoming infected, or develop into diabetic foot ulcers (DFU's) over time. Topical medications are treatments that are applied directly to the skin to treat a skin problem. There are various topical medications that may be used to address skin conditions on diabetic feet. These include medications that moisturize the skin, protect the skin from irritants, reduce itchiness, decrease pain, disinfect wounds and aid wound healing. If you have DFU's or other skin problems on your feet a podiatrist can help to find the correct treatment for you.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with the foot specialists from Podiatry Associates of Belleville. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Belleville, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Possible Symptoms of Cracked Heels
Wearing flip flops frequently may lead to the skin on the heels becoming dry, causing the condition known as cracked heels. Additionally, cracked heels may form from standing on hard surfaces for the majority of the day, or from having specific medical conditions. These conditions may consist of diabetes, obesity, eczema, and psoriasis. Research has indicated it may help to incorporate zinc and omega-3 into your diet which can be accomplished by taking vitamins. Some of the symptoms that are associated with cracked heels can include peeling skin, bleeding cracks, and the affected area may be red and itchy. If you are experiencing any signs of cracked heels please schedule a consultation with a podiatrist who can effectively treat this ailment.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact the foot specialists from Podiatry Associates of Belleville. Our doctors can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our office located in Belleville, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.